Male Infertility – Diagnosis
Diagnosis of Male Infertility
The first step a patient should take, in order to correctly diagnose their infertility is to go through a check-up that has the following aims:
- Accurate identification and confirmation of the disease.
- Assessment of the severity of the disease.
- Clarification of all existing causes & symptoms.
- Analysis of previously diagnosed accompanying diseases of the patient’s urogenital system (as they could be potential causes).
- Assessment of the reversibility of the disease.
The check-up for infertility should be detailed and the problem should be investigated in depth, as there are many different potential causes, some of which may be more subtle than the others. Tests should include:
- Clinical Examination & Medical History
- Semen Analysis
- Ultrasound of the scrotum
- Transrectal Ultrasound
- Hormonal exams
- Genetic tests
- Testicular biopsy
- Check-up for antispermatic antibodies
- Outline of spermatic tone
- Tests for sperm functionality
Clinical Examination & Medical History
A clinical examination when investigating male infertility must include:
- Checks of the genital organs (i.e. penis, epididymis, testicles, prostate gland, seminal vesicles). Mainly, the doctor should be looking for inflammations or signs of inflammations, but also for other diseases in those organs.
- Whether the patient is taking any medications.
- A record of the patient’s sexual habits.
- Whether or not the patient’s sexual development was normal.
- If there were problems with low hormone secretion or the patient’s testosterone function which resulted in symptoms such as lack of body and facial hair, or mikrofalia (small penis).
Semen Analysis
This is an important test for the diagnosis of infertility. A sample of sperm is taken (usually by masturbation), which is then poured into a clean sterile container (typically in a urine collector). A detailed analysis of the semen characteristics is done at the lab and checks for:
- Amount of liquid in the sample
- pH of the sperm
- Number of spermatozoa
- Morphology of sperm
- Sperm mobility
- Presence of inflammatory elements
The analysis of semen can show different results at different time intervals. When the analysis doesn’t fall within the normal parameters, a repetition of the examination must take place. In general, patients should have at least two semen examinations with a time difference of about 3-4 weeks between them.
Ultrasound of the scrotum
The is a detailed inspection of the ultrasound images of the epididymis, testicular and vascular component for any:
- Signs of chronic epididymal inflammation
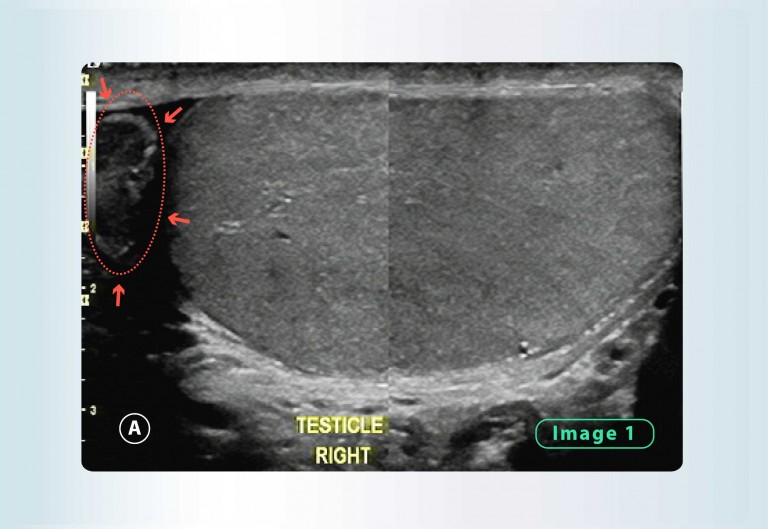
Figure 1: Ultrasound of the head epididymis. We can see chronic occult epididymitis with hypoechoic areas on the head of the epididymis, which always stems from chronic inflammation in the prostate.
- Changes in the testicles
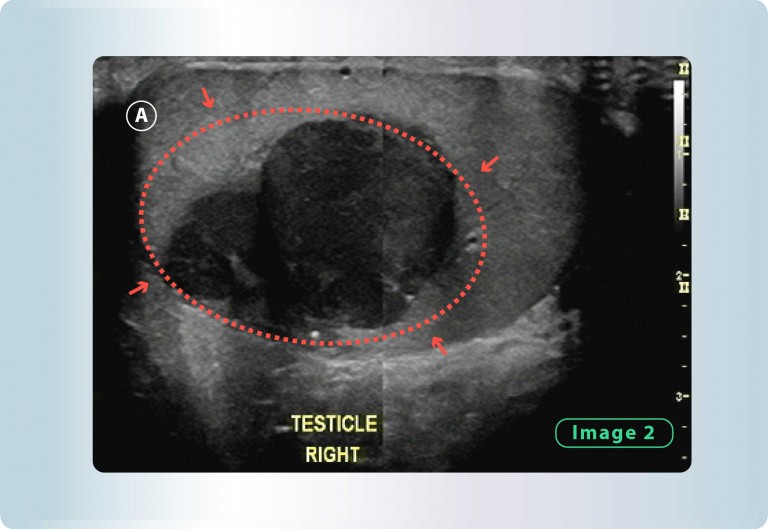
Figure 2: In this ultrasound we can see a large hypoechoic area, which actually is a tumour. This obviously can cause infertility issues.
- Presence of varicoceles and the evaluation of its extent.
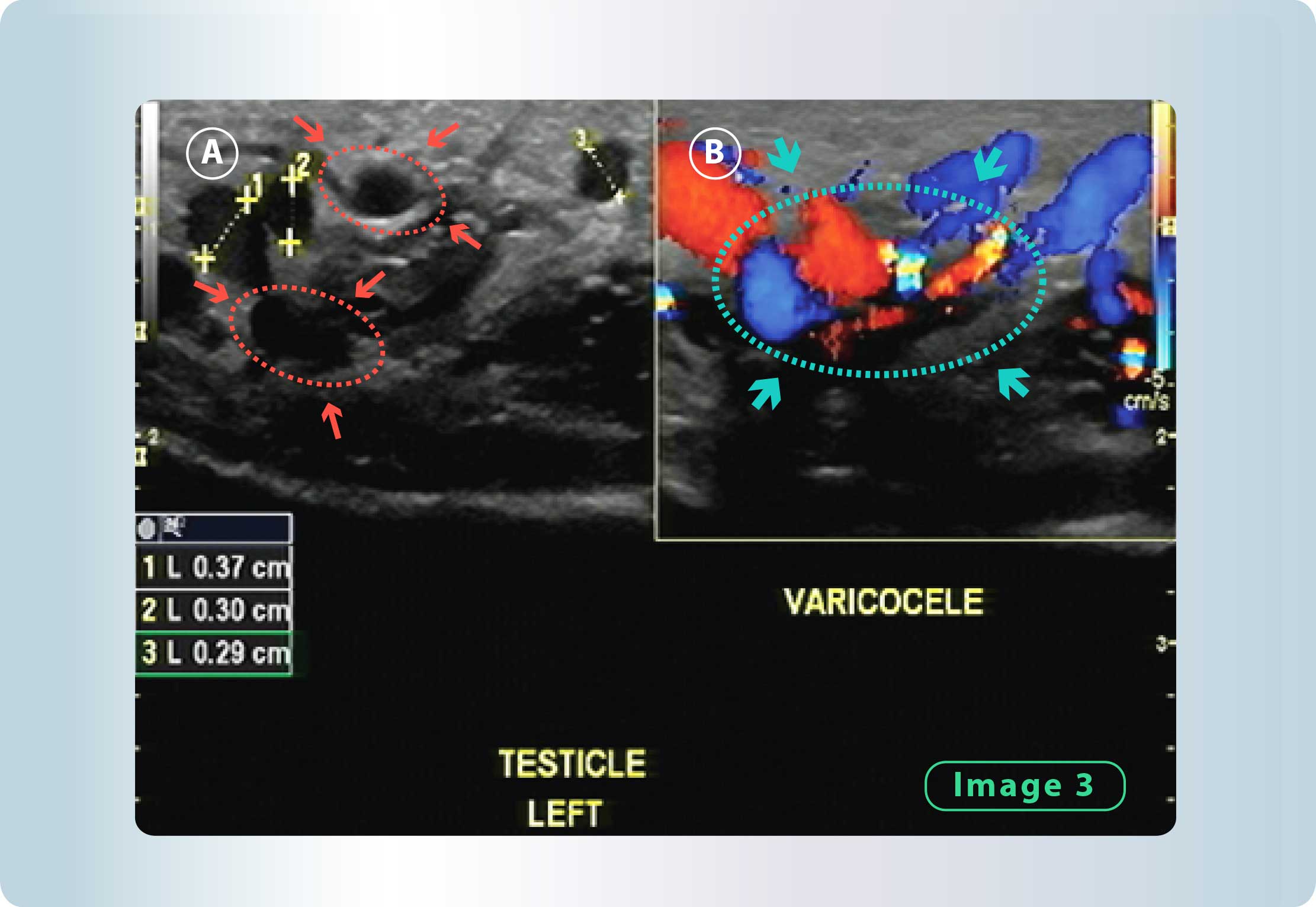
Figure 3: Ultrasound indicating Varicocele. We can see dilated veins (A) and (B), where B shows retrograded blood flow (through the venous Doppler scan). A) In the testes ultrasound, we can see dilated veins. B) High-resolution colour Doppler ultrasound, we see blood flowing in the reverse direction with Valsalva.
- Presence of cystic lesions of the epididymal head
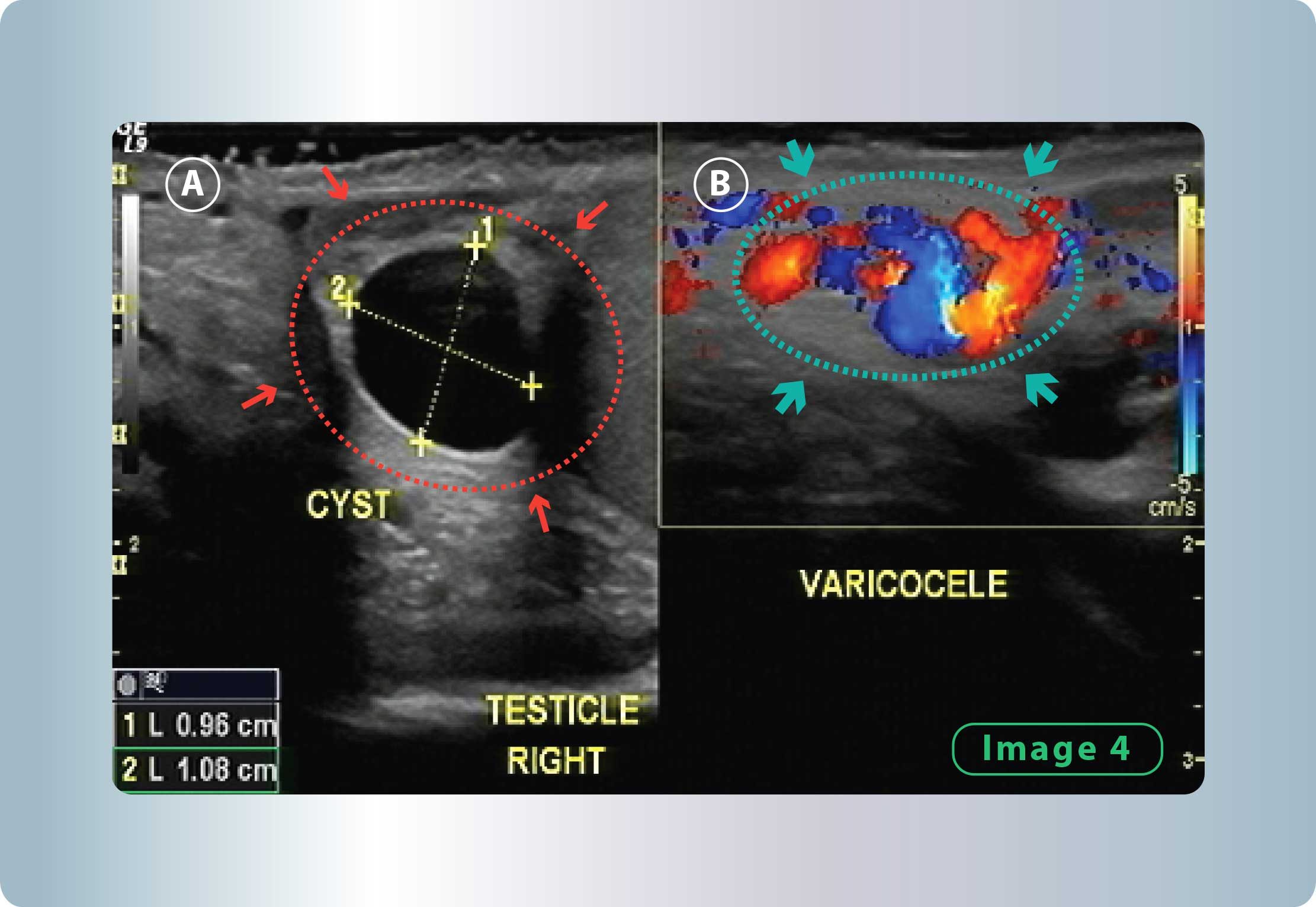
Figure 4: A) Spermatocele / Cystic Lesion of the Epididymal head. Spermatoceles stem from blocked tubes that emerge from the testicle towards the epididymis, which transport the spermatozoa. This blockage happens from the epididymis and has prostatitis as its root cause. B) Colour Doppler Ultrasonography with retrograde blood flow, indicating varicocele.
Transrectal Ultrasound
The Transrectal Ultrasound (TRUS) is a specialized diagnostic tool which enables a significantly more detailed investigation of the:
- Prostate
- Seminal Vesicles
- Ejaculatory tubes
- Control of the function of the cysteo-urethral opening mechanism (images taken during urination)
A Urologist who has additionally specialised in TRUS examinations can derive a vast amount of data during a diagnosis, such as:
- The presence of inflammatory changes in the seminal vesicles.
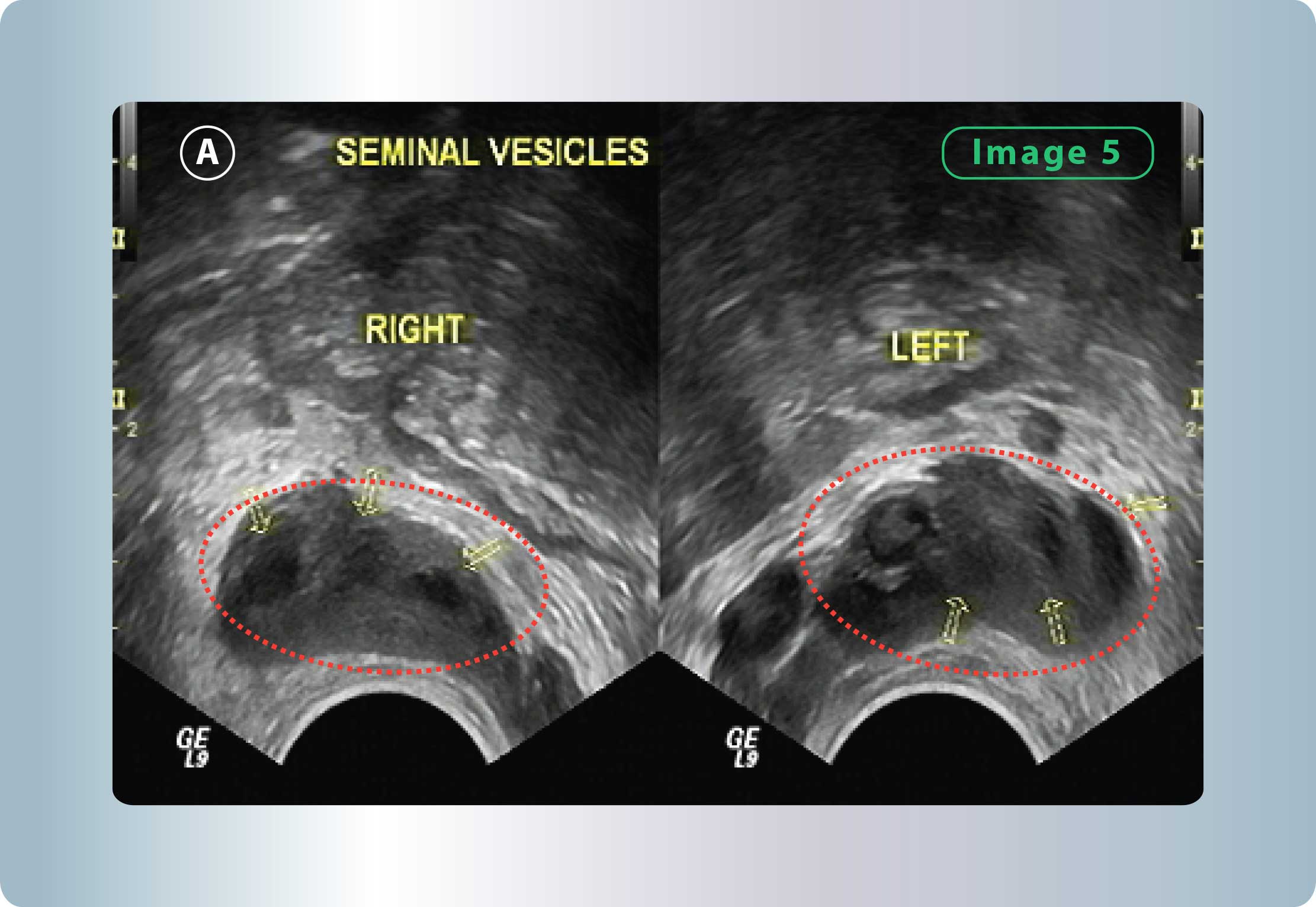
Figure 5: Seminal Vesiculitis with increased volume of the seminal vesicles and dilated “seminal compartments” (similar to a honeycomb shape). This happens due to microbes, which of course originate from the inflammation in the prostate.
- Lithiasis along the ejaculatory ducts.
- Signs of microlithiasis in the paraurethral prostatic zone.
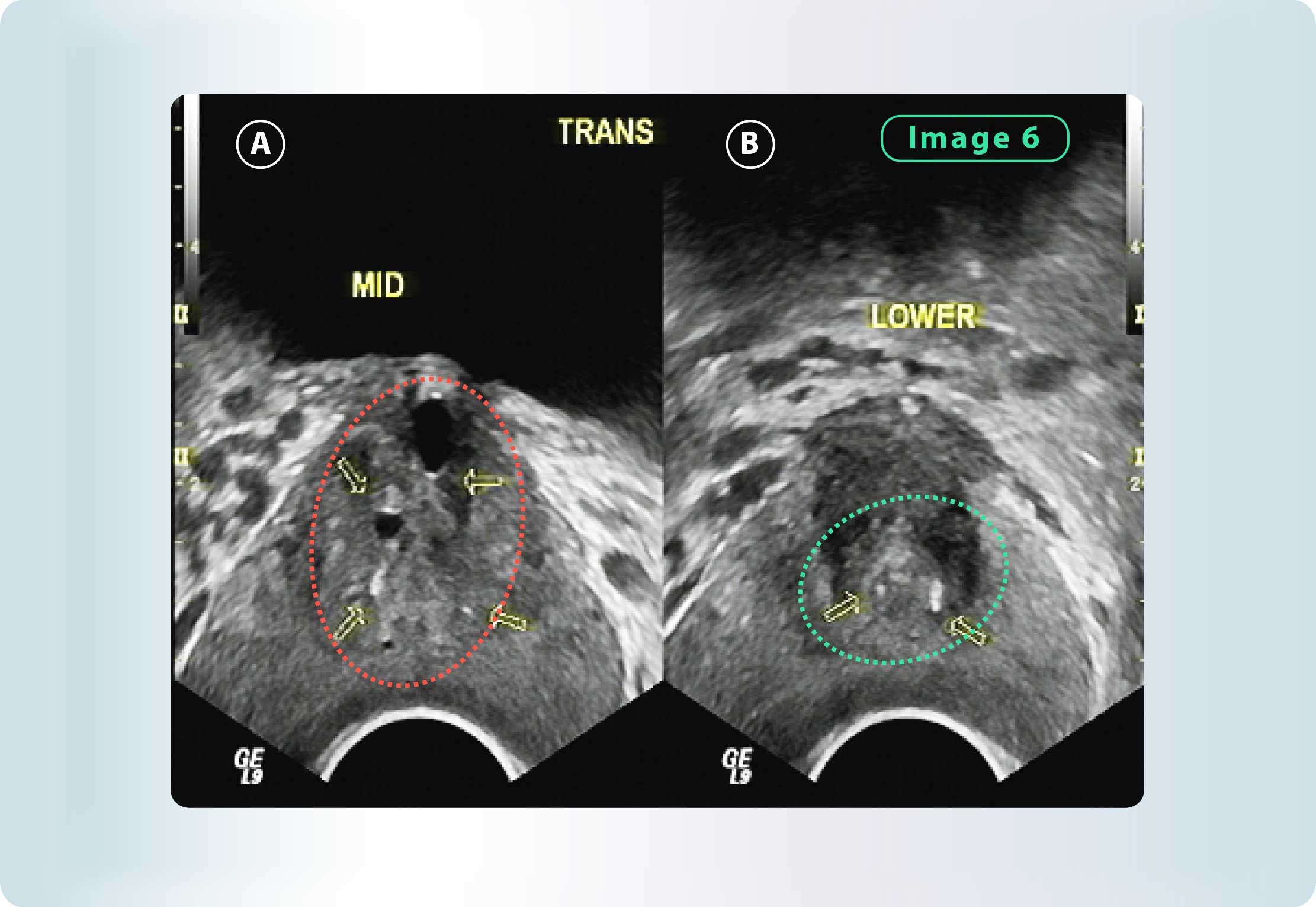
Figure 6: A) Microlithiasis in the paraurethral prostetic zone B) Lithiasis of the ejaculatory ducts at the level of verum montanum.
- Hypoechoic inflammatory areas with increased vascularity in the dynamic Doppler in the prostate peripheric parenchyma.
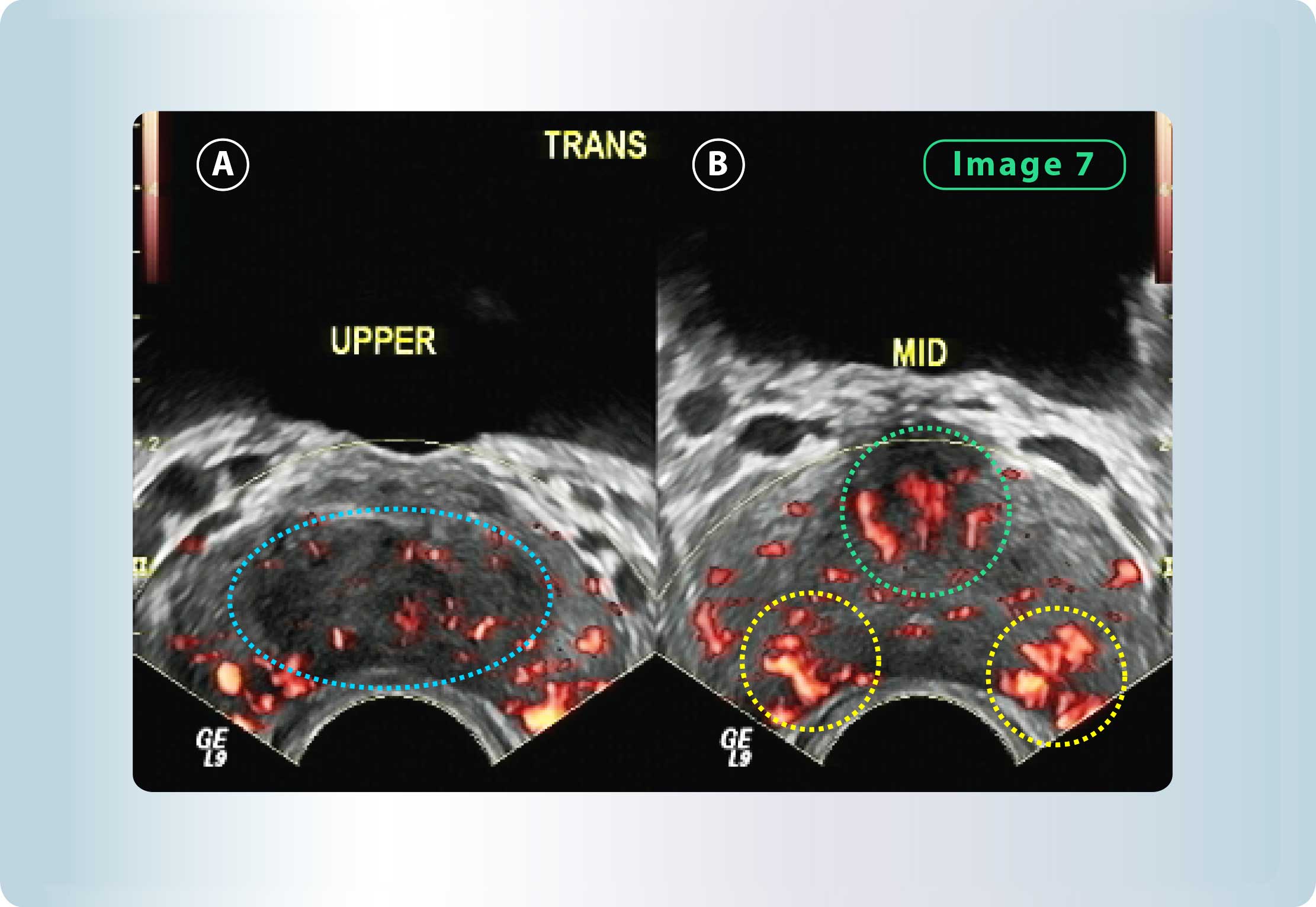
Figure 7: A) Large geographic, hypoechoic areas, which indicate, inflammation in the prostate B) Power Doppler demonstrating increased vascularity (i.e. the red spots in the image) in multiple hypo-echoic areas of inflammation.
Overall, the transrectal ultrasound is a very important tool when diagnosing male infertility as, in the hands of the skilled urologist, it shows a detailed state of:
- Almost all the organs that the sperm passes through.
- All the areas where the production of spermatic elements takes place, such as the seminal vesicles and prostatic fluid.
Hormonal determination
The hormones of the central and peripheral levels such as:
- Hypothalamus (LHRH)
- Anterior pituitary (FSH & LH)
- Testicles (TESTOSTERONE)
play an important role in sexual development and the production of sperm. A number of infertility problems may be due to factors which affect hormonal secretions and these require the relevant examinations.
Genetic tests
We proceed with genetic testing when we suspect that infertility is due to hereditary problems. This usually happens when sperm concentration is very low. A blood test may show a very slight difference/variation with the Y chromosome.
Testicular biopsy
This can be done either by using a needle or through open surgery by taking a sample of testicular tissue. We proceed to this examination when there are no indications of sperm in the semen and the level of hormones remains within normal levels. The goal is to determine if there is indeed a problem during sperm production vs. a problem during sperm transportation.
Check-up for antispermatic antibodies
This is done in order to investigate the presence of antibodies, which when created, prevent the sperm function and fertilization. This can be a result of:
- Chronic urogenital inflammation such as chronic prostatitis.
- Ligation or cross-sections of vas deferens for those who resort to this solution for fertility control.
Outline of spermatic tone
This is usually done when we suspect that there is an obstructive problem, at the height of the vas deferens.
Specialised tests of sperm functionality
These are often used to demonstrate:
- Quality of sperm movement after ejaculation.
- Effectiveness in approaching the egg.
- Potential problems in the union and penetration of sperm into the egg/ovary.
